WHAT IS THIS CANCER ALL ABOUT
Cancer is the uncontrolled growth of abnormal cells , while normal cells reproduce and develop into healthy tissue, abnormal cells reproduce faster and never grow into normal tissue. Lumps of cancer cells (tumours) then form and grow interfering with how the body functions, cancer cells can then spread from the tumour into the bloodstream, where they can spread to other organs.
POSITIVE THOUGHTS
NEVER GIVE UP in 1993 I was a reasonably fit guy, 54 yrs old with a young family and diagnosed with terminal (2 to 3 months) very fast spreading small cell lung cancer. I stubbornly decided to go down fighting and I asked for the strongest treatment available and was told that the chemo was so strong it could kill me before the cancer did. I was due to take 6 doses of chemo but stopped it after the fourth as I had nothing left and couldn’t take anymore. One year later I was back at work. Since 2000, have had ongoing surgeries and treatments, for basal cell carcinoma. In 2007, diagnosed with non small cell lung cancer and received surgery (lower left lung lobectomy). Then in September 2012 diagnosed with oesphageal cancer. Presently undergone chemo to reduce four tumours before surgery to remove them in January 2013.
In my lengthy life experiences with cancer and involvement in our local support group as a founder member, I have found that doctors give a general prognosis which is a likelihood guesstimate, based on their cancer experiences and data, Sadly people like myself are the not too often, very fortunate exceptions. Over the years I have on occasion heard a few cancer stories from people diagnosed as terminal and then proceeding to surprise the medical profession with their longevity. Not enough to give anyone positive hope, but enough to indicate that for the fighter. There can sometimes be a very hard earned reward.
Robert Lowe ( Cancer Survivor)
LATEST GOOD NEWS
People are living longer with and after a cancer diagnosis, making survivorship clinics and programmes - as well as official guidelines and practices governing the care of survivors - an important emerging component of modern cancer care. It can occasionally be cured and even if deemed incurable or inoperable, with constantly improving new modern management treatments and techniques, there are increasingly, ever improving rates of quality survival. We live in a world full of growing promise, in a time when we can communicate around the globe with the touch of a button, connect with long-lost loved ones in minutes, and can identify the body’s smallest components with technology that our parents couldn’t even imagine. We are closer than ever to understanding and defeating cancer. For those of us impacted deeply by this disease there is ever growing hope. There are many things for which to be thankful. We know so much more about how cancer works – and how it doesn’t – than at any other point in history, and we’re using this knowledge to make real progress. The battle continues, but the tide is turning and the future is looking good.
NEVER GIVE UP in 1993 I was a reasonably fit guy, 54 yrs old with a young family and diagnosed with terminal (2 to 3 months) very fast spreading small cell lung cancer. I stubbornly decided to go down fighting and I asked for the strongest treatment available and was told that the chemo was so strong it could kill me before the cancer did. I was due to take 6 doses of chemo but stopped it after the fourth as I had nothing left and couldn’t take anymore. One year later I was back at work. Since 2000, have had ongoing surgeries and treatments, for basal cell carcinoma. In 2007, diagnosed with non small cell lung cancer and received surgery (lower left lung lobectomy). Then in September 2012 diagnosed with oesphageal cancer. Presently undergone chemo to reduce four tumours before surgery to remove them in January 2013.
In my lengthy life experiences with cancer and involvement in our local support group as a founder member, I have found that doctors give a general prognosis which is a likelihood guesstimate, based on their cancer experiences and data, Sadly people like myself are the not too often, very fortunate exceptions. Over the years I have on occasion heard a few cancer stories from people diagnosed as terminal and then proceeding to surprise the medical profession with their longevity. Not enough to give anyone positive hope, but enough to indicate that for the fighter. There can sometimes be a very hard earned reward.
Robert Lowe ( Cancer Survivor)
LATEST GOOD NEWS
People are living longer with and after a cancer diagnosis, making survivorship clinics and programmes - as well as official guidelines and practices governing the care of survivors - an important emerging component of modern cancer care. It can occasionally be cured and even if deemed incurable or inoperable, with constantly improving new modern management treatments and techniques, there are increasingly, ever improving rates of quality survival. We live in a world full of growing promise, in a time when we can communicate around the globe with the touch of a button, connect with long-lost loved ones in minutes, and can identify the body’s smallest components with technology that our parents couldn’t even imagine. We are closer than ever to understanding and defeating cancer. For those of us impacted deeply by this disease there is ever growing hope. There are many things for which to be thankful. We know so much more about how cancer works – and how it doesn’t – than at any other point in history, and we’re using this knowledge to make real progress. The battle continues, but the tide is turning and the future is looking good.
TALK ABOUT CANCER
CANCER RESEARCH - NURSE HELPLINE Call friendly cancer nurses freephone on 0808 800 4040
Hearing that you or your loved one has cancer can be shocking and overwhelming.There are many emotional stages that you and your loved ones experience even before a treatment plan is made and a communication plan is needed. One way to help adjust is to be sure you, your family, and your medical team have good communication and a solid understanding of each other. By learning communication tips and tools, you’ll be able to advocate for the care you desire and the support system around you will be able to clearly understand your needs and wishes.You’ll need to speak clearly and openly with your medical team.
Make sure you hear your doctor and understand what he is saying, ask questions and verify his answers to you.
Make sure your doctor hears and understands your needs and concerns as well.
Speak up, bring two lists outlining the concerns that you want addressed during your office visit. Keep one list for you and give the other list to your doctor.
Make notes on your list and encourage your doctor to make notes on his list.
Make a plan with your medical team on your diagnosis, the immediate next steps, your treatment options, your exact treatment plan, and what to do when there are side effects. You also need a plan on how and who you will communicate your needs, concerns, and wishes to. If possible, bring someone with you to your doctor’s appointments. People hear things differently, which is why it is important to write things down, verify what you are hearing, audio record the visit, and/or bring another set of ears to hear what is being relayed to you. Getting in plain writing a detailed description of your office visit and treatment plan would be ideal but it isn’t always probable or possible, so using one or more of these tools to get a clear understanding of your appointment visit and expectations will help keep you more at ease as you move forward in your treatment.
http://community.macmillan.org.uk/p/communitychat.aspx
Hearing that you or your loved one has cancer can be shocking and overwhelming.There are many emotional stages that you and your loved ones experience even before a treatment plan is made and a communication plan is needed. One way to help adjust is to be sure you, your family, and your medical team have good communication and a solid understanding of each other. By learning communication tips and tools, you’ll be able to advocate for the care you desire and the support system around you will be able to clearly understand your needs and wishes.You’ll need to speak clearly and openly with your medical team.
Make sure you hear your doctor and understand what he is saying, ask questions and verify his answers to you.
Make sure your doctor hears and understands your needs and concerns as well.
Speak up, bring two lists outlining the concerns that you want addressed during your office visit. Keep one list for you and give the other list to your doctor.
Make notes on your list and encourage your doctor to make notes on his list.
Make a plan with your medical team on your diagnosis, the immediate next steps, your treatment options, your exact treatment plan, and what to do when there are side effects. You also need a plan on how and who you will communicate your needs, concerns, and wishes to. If possible, bring someone with you to your doctor’s appointments. People hear things differently, which is why it is important to write things down, verify what you are hearing, audio record the visit, and/or bring another set of ears to hear what is being relayed to you. Getting in plain writing a detailed description of your office visit and treatment plan would be ideal but it isn’t always probable or possible, so using one or more of these tools to get a clear understanding of your appointment visit and expectations will help keep you more at ease as you move forward in your treatment.
http://community.macmillan.org.uk/p/communitychat.aspx
Important for people diagnosed with cancer
Faced with overwhelming anxiety, patients newly diagnosed with cancer can find themselves in distress, and new research recommends nurses play a key role in alleviating concerns, leading to a better quality of life for patients. Recent studies have confirmed that too many lung cancer patients and their carers never see a lung nurse. The latest National Lung Cancer Audit published by the NHS Information Centre, highlighted wide variations in the level of treatment patients receive. Only three-quarters of lung cancer patients were seen by a specialist nurse, while just 43.7% had a specialist nurse present at diagnosis. Of patients seen by a lung cancer nurse specialist, 64.8% went on to receive treatment, compared with just 30.4% of patients who did not see a specialist nurse. There are only 25 (whole time equivalent) lung cancer CNSs working in Scotland, looking after 4,000 new lung cancer patients every year. The NHS audit identified that undermanning and improved access to clinical nurse specialists needs to be addressed.
The local nurse specialist is a major player in patient and carer wellbeing. Their superb people skills enable them to explain technicalities and procedures in a more rounded easily understood way. You will find them essential in providing continuity among all the doctors and specialists who will be involved in your care. An introduction should be available to you and your carer right from the start. They are a key worker, giving advice, information, and support. They can spend more time with you, visit you at home, and be available by phone and email, to answer your questions.
Patient Power
To find out who your local nurse specialist is, ask your hospital/consultant. If you have any difficulties getting access to a nurse, or the service provided by your nurse is inconsistent or inadequate, do your bit for nurses, other patients and carers, write a complaint and hand it to your specialist. There is nothing NHS managers hate more, or will pay more attention to, than complaints.
You should expect a quick response.
http://www.nursingtimes.net/nursing-practice/clinical-specialisms/cancer/specialist-nurses-boost-care-for-lung-cancer-patients/5030101.article
http://www.medicalnewstoday.com/releases/242283.php
THINGS TO DO
On your diagnosis, demand regular access to a clinical nurse specialist and arrange for a family member or key carer to accompany you to appointments especially at the beginning.
The Day of Your Operation
Guidance provided on all required safety checks and pain management options.
http://www.facs.org/patienteducation/skills/lung/dvd04.html
Faced with overwhelming anxiety, patients newly diagnosed with cancer can find themselves in distress, and new research recommends nurses play a key role in alleviating concerns, leading to a better quality of life for patients. Recent studies have confirmed that too many lung cancer patients and their carers never see a lung nurse. The latest National Lung Cancer Audit published by the NHS Information Centre, highlighted wide variations in the level of treatment patients receive. Only three-quarters of lung cancer patients were seen by a specialist nurse, while just 43.7% had a specialist nurse present at diagnosis. Of patients seen by a lung cancer nurse specialist, 64.8% went on to receive treatment, compared with just 30.4% of patients who did not see a specialist nurse. There are only 25 (whole time equivalent) lung cancer CNSs working in Scotland, looking after 4,000 new lung cancer patients every year. The NHS audit identified that undermanning and improved access to clinical nurse specialists needs to be addressed.
The local nurse specialist is a major player in patient and carer wellbeing. Their superb people skills enable them to explain technicalities and procedures in a more rounded easily understood way. You will find them essential in providing continuity among all the doctors and specialists who will be involved in your care. An introduction should be available to you and your carer right from the start. They are a key worker, giving advice, information, and support. They can spend more time with you, visit you at home, and be available by phone and email, to answer your questions.
Patient Power
To find out who your local nurse specialist is, ask your hospital/consultant. If you have any difficulties getting access to a nurse, or the service provided by your nurse is inconsistent or inadequate, do your bit for nurses, other patients and carers, write a complaint and hand it to your specialist. There is nothing NHS managers hate more, or will pay more attention to, than complaints.
You should expect a quick response.
http://www.nursingtimes.net/nursing-practice/clinical-specialisms/cancer/specialist-nurses-boost-care-for-lung-cancer-patients/5030101.article
http://www.medicalnewstoday.com/releases/242283.php
THINGS TO DO
On your diagnosis, demand regular access to a clinical nurse specialist and arrange for a family member or key carer to accompany you to appointments especially at the beginning.
- Make sure you know who to contact if your condition deteriorates.
- Ask your GP what services are available for you in the community.
- Speak to your nurse and get in touch with social services to find out about special benefits, such as Attendance Allowance, which can be fast tracked for seriously ill people.
- Call Macmillan Cancer 0808 808 00 00 and ask to speak to a benefits advisor, or call the benefit enquiry line 0800 882 200.
- Find out if there are any cancer support groups in your area.
The Day of Your Operation
Guidance provided on all required safety checks and pain management options.
http://www.facs.org/patienteducation/skills/lung/dvd04.html
Regular exercise can help reduce the side effects of treatment. All patients getting cancer treatment should be told to do two and a half hours of physical exercise every week. Being advised to rest and take it easy after treatment is an outdated view. Research shows that exercise can reduce the risk of dying from cancer and minimise the side effects of treatment. Debilitating fatigue is a common side effect and can last for months or even years after treatment. It is a factor that not only significantly diminishes quality of life but is also associated with reduced survival.
http://www.bbc.co.uk/news/health-14417084
Patients with advanced cancer suffer from cachexia, a condition also called body-wasting or wasting syndrome, which causes significant weight loss, extreme fatigue and reduces quality of life. A study shows that higher levels of cancer-related fatigue coincide with lower levels of muscle mass. For this study, the fatigue levels, muscle mass and strength of 84 patients with newly diagnosed and inoperable lung cancer were assessed. Handgrip and quadricep strength were determined using muscle strength tests, and skeletal muscle mass was calculated using X-rays. These measures were then compared to a "brief fatigue inventory” which was found to be positively associated with body mass, weight loss, anaemia, activity level, pain, and depression. All advanced cancer patients suffer from this type of fatigue.” The study hopes these findings will encourage hospitals and health centres to launch specialized strength or aerobics training programmes that can improve muscle mass among cancer patients.
http://www.medicalnewstoday.com/releases/241432.php
Lung Cancer and Exercise?
Regular exercise is one of the best things a person can do as a cancer patient or survivor, with studies showing improvements in cardio respiratory fitness, quality of life, fatigue, and depression. However, very few studies have focused on the feasibility, safety, or efficacy of exercise in cancer patients. Is exercise safe for people with cancer? Is it beneficial? Is a long-term exercise program feasible? Yes. Yes and yes, say experts.
The Results Are In -
http://curetoday.com/index.cfm/fuseaction/article.showArticleByTumorType/id/818/tumorCategory/Lung/article_id/1429
Researchers are working to prove, with scientific certainty, that prescriptions for daily yoga or 20 minutes of walking will extend a patient's survival.
In our support group the seven longest lung cancer survivors all advocate and take regular exercise. Includes our longest survivor (myself) of both small cell (given a terminal diagnosis of 2/3 months) in 1993, for which I received chemo and radiotherapy, and then with non small cell in 2007, when I received a lower lobectomy. I along with my other fellow keep fit long term club members, are all still going strong with a pretty good quality of life, so it tends to confirm the above recommendation, don't you think?
CANCER (YOUR RIGHTS)
http://www.bbc.co.uk/health/support/carecancer_rights.shtml
http://www.bbc.co.uk/news/health-14417084
Patients with advanced cancer suffer from cachexia, a condition also called body-wasting or wasting syndrome, which causes significant weight loss, extreme fatigue and reduces quality of life. A study shows that higher levels of cancer-related fatigue coincide with lower levels of muscle mass. For this study, the fatigue levels, muscle mass and strength of 84 patients with newly diagnosed and inoperable lung cancer were assessed. Handgrip and quadricep strength were determined using muscle strength tests, and skeletal muscle mass was calculated using X-rays. These measures were then compared to a "brief fatigue inventory” which was found to be positively associated with body mass, weight loss, anaemia, activity level, pain, and depression. All advanced cancer patients suffer from this type of fatigue.” The study hopes these findings will encourage hospitals and health centres to launch specialized strength or aerobics training programmes that can improve muscle mass among cancer patients.
http://www.medicalnewstoday.com/releases/241432.php
Lung Cancer and Exercise?
Regular exercise is one of the best things a person can do as a cancer patient or survivor, with studies showing improvements in cardio respiratory fitness, quality of life, fatigue, and depression. However, very few studies have focused on the feasibility, safety, or efficacy of exercise in cancer patients. Is exercise safe for people with cancer? Is it beneficial? Is a long-term exercise program feasible? Yes. Yes and yes, say experts.
The Results Are In -
http://curetoday.com/index.cfm/fuseaction/article.showArticleByTumorType/id/818/tumorCategory/Lung/article_id/1429
Researchers are working to prove, with scientific certainty, that prescriptions for daily yoga or 20 minutes of walking will extend a patient's survival.
In our support group the seven longest lung cancer survivors all advocate and take regular exercise. Includes our longest survivor (myself) of both small cell (given a terminal diagnosis of 2/3 months) in 1993, for which I received chemo and radiotherapy, and then with non small cell in 2007, when I received a lower lobectomy. I along with my other fellow keep fit long term club members, are all still going strong with a pretty good quality of life, so it tends to confirm the above recommendation, don't you think?
CANCER (YOUR RIGHTS)
http://www.bbc.co.uk/health/support/carecancer_rights.shtml
TREATMENTS
Are determined by the patient’s physical fitness and the type and spread of the cancer.
http://www.nhs.uk/conditions/cancer-of-the-lung/pages/treatment.aspx
BBC HORIZON DEFEATING CANCER
Documentary looking at three state-of-the-art interventions for aggressive cancers
http://www.youtube.com/watch?v=7sB2G4vm1uk
Diagnostic Tools: Imaging
Diagnostic imaging can play a big role throughout all phases of the cancer journey. These tests and scans are used to make pictures of areas inside the body, which can help doctors identify and locate disease, guide certain
treatment modalities, monitor treatment response, and spot recurrences during follow-up.
http://www.cancercompass.com/cancer-news/article/diagnostic-tools-imaging-101?c=NL20121003
Diagnostic imaging can play a big role throughout all phases of the cancer journey. These tests and scans are used to make pictures of areas inside the body, which can help doctors identify and locate disease, guide certain
treatment modalities, monitor treatment response, and spot recurrences during follow-up.
http://www.cancercompass.com/cancer-news/article/diagnostic-tools-imaging-101?c=NL20121003
RADIOTHERAPY
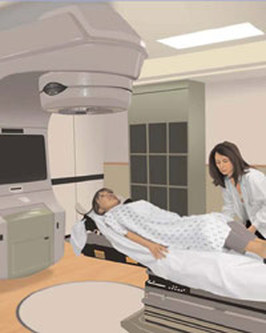
Radiotherapy is a general term for the treatment of cancer with x-rays. It works by killing cancer cells and is often used on its own to treat lung cancer. It may also be given as part of a combined treatment with surgery and /or chemotherapy
http://www.nhs.uk/Conditions/Radiotherapy/Pages/Introduction.aspx
Radiation therapy is one of the many tools used to combat cancers. Radiation treatments utilize high-energy waves such as x-rays to kill cancer cells. Radiation can be used alone or in conjunction with other treatments (e.g. chemotherapy and surgery) to cure or stabilize cancer. Like other therapies, the choice to use radiation to treat a particular cancer depends on a wide range of factors. These include, but are not limited to, the type of cancer, the physical state of the patient, the stage of the cancer, and the location of the tumour.
http://www.youtube.com/watch?v=S-WIQhM43ng
http://www.youtube.com/watch?v=Hv1Of2_drRc
http://www.cancerquest.org/radiation-therapy-introduction.html
http://www.nhs.uk/Conditions/Radiotherapy/Pages/Introduction.aspx
Radiation therapy is one of the many tools used to combat cancers. Radiation treatments utilize high-energy waves such as x-rays to kill cancer cells. Radiation can be used alone or in conjunction with other treatments (e.g. chemotherapy and surgery) to cure or stabilize cancer. Like other therapies, the choice to use radiation to treat a particular cancer depends on a wide range of factors. These include, but are not limited to, the type of cancer, the physical state of the patient, the stage of the cancer, and the location of the tumour.
http://www.youtube.com/watch?v=S-WIQhM43ng
http://www.youtube.com/watch?v=Hv1Of2_drRc
http://www.cancerquest.org/radiation-therapy-introduction.html
CHEMOTHERAPY
Chemotherapy is a term for the treatment of cancer using drugs. Patients with different types of lung cancer are likely to receive different strengths and combinations of chemotherapy drugs. After discussing your treatment options with you, your doctor will decide which chemotherapy drugs are most suitable.
http://www.nhs.uk/conditions/chemotherapy/pages/definition.aspx
INTRODUCTION TO CHEMOTHERAPY CANCER TREATMENT
The term chemotherapy, or chemo, refers to a wide range of drugs used to treat cancer. These drugs usually work by killing dividing cells. Since cancer cells have lost many of the regulatory functions present in normal cells, they will continue to attempt to divide when other cells do not. This trait makes cancer cells susceptible to a wide range of cellular poisons. The chemotherapy agents work to cause cell death in a variety of ways. Some of the drugs are naturally occurring compounds that have been identified in various plants and some are man-made chemicals.
VIDEO:
http://www.youtube.com/watch?v=p1xLMxIEjKw
http://www.cancerquest.org/chemotherapy-introduction.html?gclid=CNifnrjJirMCFe7MtAodE28AWA#
http://www.nhs.uk/conditions/chemotherapy/pages/definition.aspx
INTRODUCTION TO CHEMOTHERAPY CANCER TREATMENT
The term chemotherapy, or chemo, refers to a wide range of drugs used to treat cancer. These drugs usually work by killing dividing cells. Since cancer cells have lost many of the regulatory functions present in normal cells, they will continue to attempt to divide when other cells do not. This trait makes cancer cells susceptible to a wide range of cellular poisons. The chemotherapy agents work to cause cell death in a variety of ways. Some of the drugs are naturally occurring compounds that have been identified in various plants and some are man-made chemicals.
VIDEO:
http://www.youtube.com/watch?v=p1xLMxIEjKw
http://www.cancerquest.org/chemotherapy-introduction.html?gclid=CNifnrjJirMCFe7MtAodE28AWA#
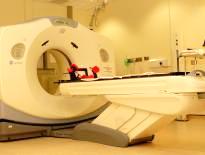
CT SCAN
http://www.youtube.com/watch?feature=player_embedded&v=Tx-0emi4m8s#!
MRI SCAN
http://www.youtube.com/watch?v=lZVYF2zgmII
http://www.youtube.com/watch?feature=player_embedded&v=Tx-0emi4m8s#!
PET SCAN
http://www.youtube.com/watch?v=9JISCohidOg
http://www.youtube.com/watch?feature=player_embedded&v=Tx-0emi4m8s#!
MRI SCAN
http://www.youtube.com/watch?v=lZVYF2zgmII
http://www.youtube.com/watch?feature=player_embedded&v=Tx-0emi4m8s#!
PET SCAN
http://www.youtube.com/watch?v=9JISCohidOg
SURGERY
Surgery is frequently used to remove cancerous growths or obtain small samples of tissue for examination. For several types of cancer, surgical removal of a tumour may be sufficient to cure the patient. The likelihood of a surgical cure is dependent on the size, location, and stage of the disease. When removing a tumour the surgeon will try to remove as much of the tumour as possible. The tissue removed from the patient will often be examined by a pathologist for signs of tumour cells near the edge of the incision. This is to ensure that all detectable cancer cells have been removed. If no cancer cells are visible in the tissue surrounding the excised tissue, the specimen may be said to have 'clean margins'. This refers to the fact that all visible tumour cells have been removed. Using microscopes, pathologists can look very closely at the removed tissue to see if any cancer cells may have been left behind. If there are areas around the perimeter of the excised tissue that do not have a margin of normal cells then some cancerous cells may have been left behind. In this case the surgeon may go back to remove more tissue surrounding the tumour site. Surgery is often used in combination with radiation and/or chemotherapy. The choice of treatments depends on the type, location and size of the tumour.
*Wedge Resection Removes small nodules and is the procedure of choice if your physical condition will not allow surgery that is more extensive.
*Lobectomy (Lobe removal) Performed when lung cancer is confined to a single lobe of your lung.
*Pneumonectomy A pneumonectomy is a procedure that is used to remove a lung because it has a cancerous tumour. It is used to relieve some or all of the lung cancer symptoms that a person is feeling. A pneumonectomy can help keep your health from getting worse, and it may provide the best chance for curing your disease.
*Lobectomy (Lobe removal) Performed when lung cancer is confined to a single lobe of your lung.
*Pneumonectomy A pneumonectomy is a procedure that is used to remove a lung because it has a cancerous tumour. It is used to relieve some or all of the lung cancer symptoms that a person is feeling. A pneumonectomy can help keep your health from getting worse, and it may provide the best chance for curing your disease.
STAGING
If the doctor makes a cancer diagnosis, he or she will want to determine the stage (or extent) of the disease. Staging is conducted to find out whether lung cancer has spread and, if so, to what parts of the body.
http://www.nhs.uk/chq/pages/3169.aspx?categoryid=96&subcategoryid=226
http://cancerhelp.cancerresearchuk.org/type/lung-cancer/treatment/lung-cancer-staging
http://www.nhs.uk/chq/pages/3169.aspx?categoryid=96&subcategoryid=226
http://cancerhelp.cancerresearchuk.org/type/lung-cancer/treatment/lung-cancer-staging
WHAT IS A CLINICAL TRIAL?
Clinical trials are carefully controlled research studies in which patients may participate. These studies may test whether a new treatment is safe and how well it works in patients, or look at new ways to diagnose or prevent a disease. Clinical trials may also focus on refinements to existing standard therapies. Most of the advances in cancer therapy have resulted from the participation of patients in clinical trials.
http://nccn.com/clinical-trials/855.html
http://www.nhs.uk/Conditions/Clinical-trials/Pages/clinical-trial.aspx?Condition=lung+cancer
http://nccn.com/clinical-trials/855.html
http://www.nhs.uk/Conditions/Clinical-trials/Pages/clinical-trial.aspx?Condition=lung+cancer
MAINTENANCE THERAPY
Maintenance therapy refers to treatment that is given after initial treatment but before cancer progression. It is a relatively new approach to lung cancer treatment. Drugs that have been approved for maintenance therapy in selected patients include Alimta® (pemetrexed) and Tarceva® (erlotinib). For patients who are candidates for maintenance therapy, the approach has been shown to delay cancer progression and improve overall survival.
http://lungcancer.about.com/od/treatmentoflungcancer/a/Maintenance-Therapy-For-Lung-Cancer.htm
Maintenance therapy refers to treatment that is given after initial treatment but before cancer progression. It is a relatively new approach to lung cancer treatment. Drugs that have been approved for maintenance therapy in selected patients include Alimta® (pemetrexed) and Tarceva® (erlotinib). For patients who are candidates for maintenance therapy, the approach has been shown to delay cancer progression and improve overall survival.
http://lungcancer.about.com/od/treatmentoflungcancer/a/Maintenance-Therapy-For-Lung-Cancer.htm
DEPRESSION
A cancer diagnosis is often accompanied by varied depths of depression.
How can you tell if you have depression?
New research suggests mental health issues are more common than previously thought, but that people aren't getting the help they need. It seems that few of us diagnose ourselves as depressed. "People often come to see me not with a mental health problem, but with the impact it has on their lives," says Dr Andrew Jones, a sessional GP in Surrey and head of clinical engagement at the BMJ Group. "They'll be struggling at work, not sleeping, drinking too much alcohol or getting headaches. But they know somewhere that it's not really the problem."
This may be because it is hard to recognise your own depression. "We all know what it is like to feel sad when something bad happens but with depression the feelings go on for much longer and you don't bounce back," says Dr Jim Bolton, a psychiatrist in south-west London. "If you think you are depressed or anxious you should see your GP. It won't be an uncomfortable conversation." In fact GPs can detect depression by running through a short questionnaire, the PHQ-9, in which you are asked if you are feeling tired, having difficulty concentrating or if you have thought about ending your life.
http://www.guardian.co.uk/lifeandstyle/2012/jun/24/right-treatment-for-depression
http://www.nhs.uk/conditions/depression/pages/introduction.aspx
How can you tell if you have depression?
New research suggests mental health issues are more common than previously thought, but that people aren't getting the help they need. It seems that few of us diagnose ourselves as depressed. "People often come to see me not with a mental health problem, but with the impact it has on their lives," says Dr Andrew Jones, a sessional GP in Surrey and head of clinical engagement at the BMJ Group. "They'll be struggling at work, not sleeping, drinking too much alcohol or getting headaches. But they know somewhere that it's not really the problem."
This may be because it is hard to recognise your own depression. "We all know what it is like to feel sad when something bad happens but with depression the feelings go on for much longer and you don't bounce back," says Dr Jim Bolton, a psychiatrist in south-west London. "If you think you are depressed or anxious you should see your GP. It won't be an uncomfortable conversation." In fact GPs can detect depression by running through a short questionnaire, the PHQ-9, in which you are asked if you are feeling tired, having difficulty concentrating or if you have thought about ending your life.
http://www.guardian.co.uk/lifeandstyle/2012/jun/24/right-treatment-for-depression
http://www.nhs.uk/conditions/depression/pages/introduction.aspx
POSITIVITY @ EXERCISE
The biggest natural aids to beating cancer. Life is what you make it.
GOOD LUCK!
The views expressed on this free website are those of the author a long term dual survivor of both small and non small cell lung cancer. The information published is intended to help increase awareness and is not a substitute for professional medical advice, diagnosis, or treatment. Always consult with a physician or other health care professional.
GOOD LUCK!
The views expressed on this free website are those of the author a long term dual survivor of both small and non small cell lung cancer. The information published is intended to help increase awareness and is not a substitute for professional medical advice, diagnosis, or treatment. Always consult with a physician or other health care professional.
TUTORIALS
CLICK ON TOPIC
Medline
VICC
BBC Health
FIND A CLINICAL TRIAL
FIND A BENEFITS ADVISOR
FIND A LOCAL SUPPORT GROUP
Medline
VICC
BBC Health
FIND A CLINICAL TRIAL
FIND A BENEFITS ADVISOR
FIND A LOCAL SUPPORT GROUP


